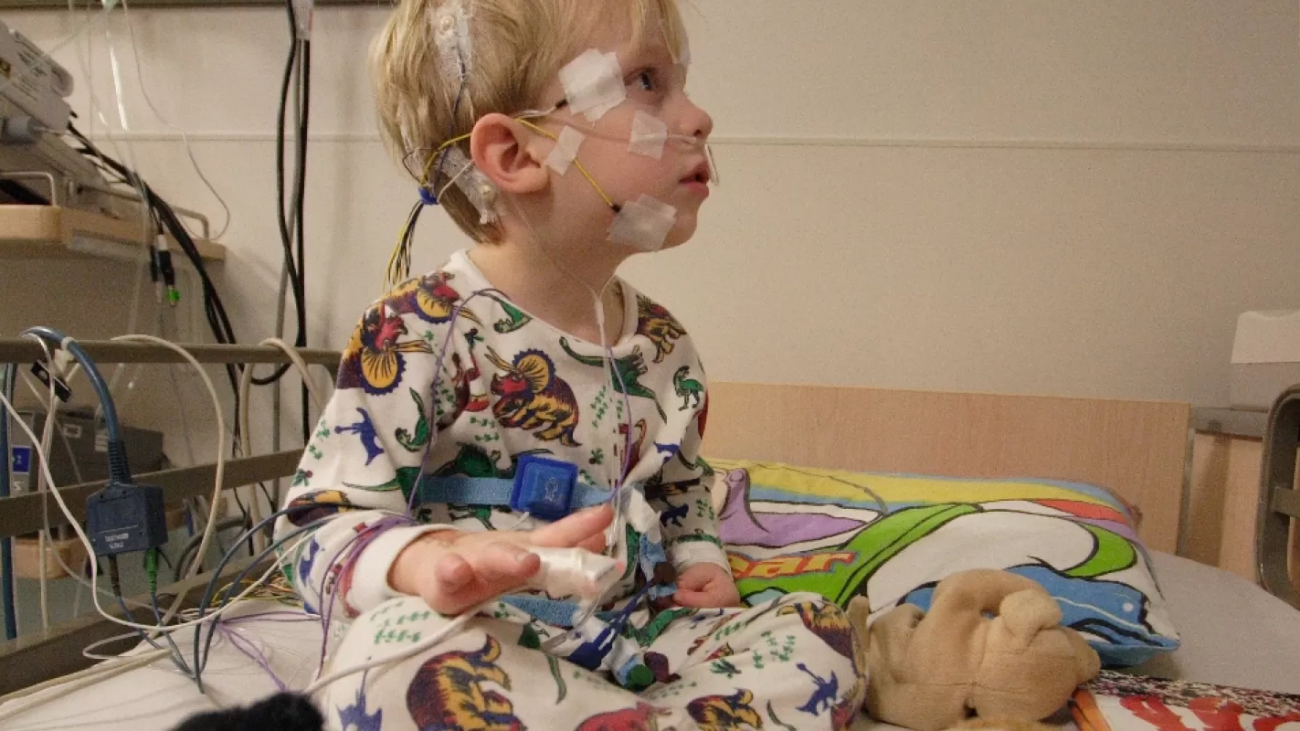
A sleep study in Adelaide helps clinicians figure out why someone is not sleeping well, snoring loudly, or feeling exhausted during the day. It records key body signals overnight so a sleep physician can diagnose issues like obstructive sleep apnoea, insomnia patterns, or movement disorders.
For many people, the hardest part is not the test itself. It is knowing what to expect, what it can and cannot show, and how to prepare so the results are useful when considering a sleep study Adelaide and ensuring the process provides accurate insights into sleep health.
What is a sleep study, and what does it measure?
A sleep study records sleep and breathing to identify disruptions that someone cannot see at home. It typically tracks airflow, oxygen levels, breathing effort, heart rate, body position, and snoring.
In more comprehensive studies, it can also measure brain activity and sleep stages. That extra detail helps clinicians separate problems such as apnoea, insomnia, and unusual movements during sleep.
Who should consider a sleep study in Adelaide?
They should consider a sleep study if they have symptoms that suggest a sleep disorder that needs confirmation. Common triggers include loud snoring, choking or gasping at night, witnessed pauses in breathing, morning headaches, or persistent daytime sleepiness.
It can also be relevant for people with high blood pressure, type 2 diabetes, or weight gain where sleep apnoea is suspected. Some may be referred because of fatigue-related driving risk or work safety concerns. You may also visit https://www.healthdirect.gov.au/type-2-diabetes to get more kowledge about type 2 diabetes.
How do they know if they need a home study or an in-lab study?
The best option depends on symptoms, medical history, and what the clinician needs to rule in or out. Home sleep studies are often used when obstructive sleep apnoea is strongly suspected and there are no complex medical issues.
In-lab studies are more suitable if they have significant heart or lung disease, suspected central sleep apnoea, unusual movements, possible narcolepsy, or when prior testing was unclear. In-lab testing can also capture more signals and sleep stages.
What happens during a home sleep study?
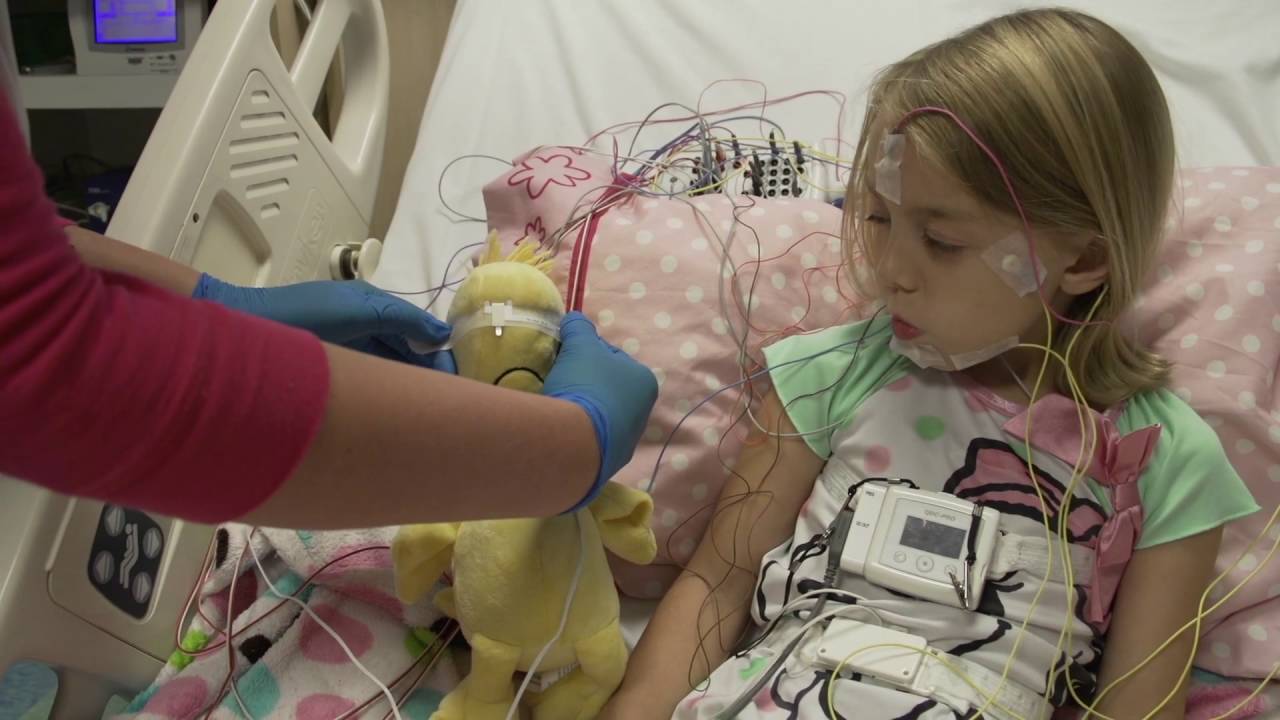
A home sleep study usually involves a small portable device they wear for one night. It commonly includes a nasal cannula to measure airflow, a finger probe for oxygen, and belts around the chest or abdomen for breathing effort.
They set it up before bed, sleep in their own environment, then return the equipment the next day. Because it is done at home, the night can feel more normal, though sensors can still take a little getting used to.
What happens during an in-lab sleep study?
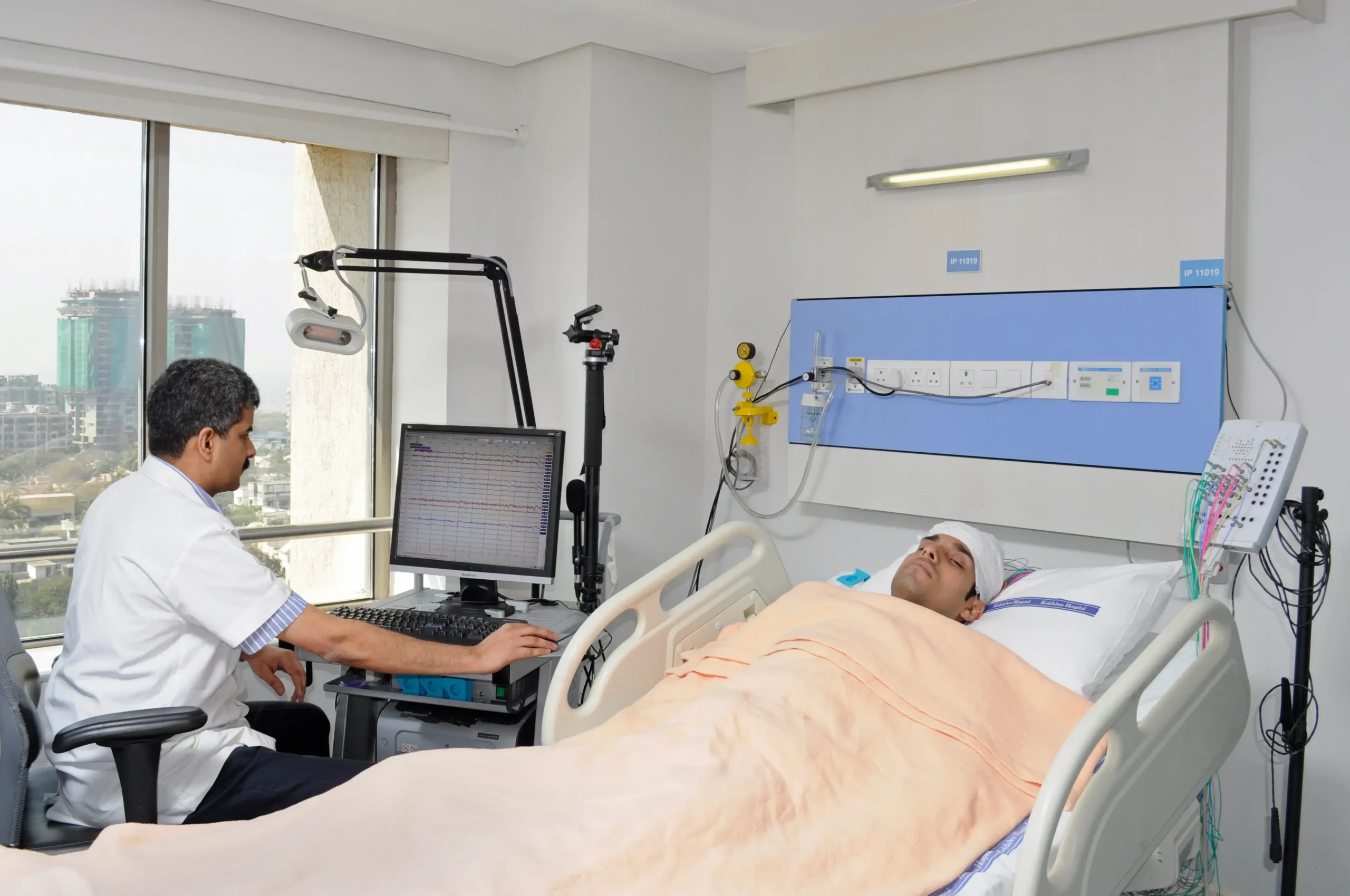
In-lab studies are done overnight in a sleep clinic where trained staff monitor signals throughout the night. They are fitted with sensors that may include scalp electrodes for sleep stages, eye movement sensors, muscle sensors, breathing measures, and oxygen monitoring. Learn more about overnight diagnostic sleep studies.
Staff can troubleshoot sensors if they fall off and may add extra monitoring if needed. The environment is designed for sleep, but it still differs from home, which can slightly affect how quickly they fall asleep.
How should they prepare the day of the sleep study?
They should aim for a typical day so the test reflects normal sleep. Most clinics recommend avoiding naps, limiting caffeine later in the day, and avoiding alcohol because it can worsen snoring and apnoea.
They should follow medication instructions from the referring clinician and bring their usual bedtime items if attending in-lab. Clean, dry skin can help sensors stick properly, so heavy lotions and hair products are best avoided.
What should they bring if the sleep study is in a clinic?
They should bring comfortable sleepwear, toiletries, and any nighttime medications they normally take. If they use a mouthguard or other sleep device, they should bring it unless told otherwise.
Many people also bring a book or headphones to wind down. They can ask ahead about parking, check-in times, and whether they can eat a light snack before settling in.
What do sleep study results usually show?
Results usually show whether breathing is repeatedly interrupted during sleep and how severe those interruptions are. For suspected sleep apnoea, clinicians often focus on indices that count breathing events and how low oxygen levels drop.
They may also comment on snoring, sleep position effects, heart rate changes, and sleep quality. For in-lab studies, results can include sleep stage distribution and arousal patterns.
How long does it take to get results and next steps?
It often takes days to a couple of weeks, depending on the clinic and whether a sleep physician needs to review a detailed report. Once results are in, they may be offered a follow-up appointment to explain what was found.
If sleep apnoea is diagnosed, next steps can include CPAP therapy, oral appliances, weight management support, positional therapy, or referral to an ENT specialist. If apnoea is not present, the clinician may investigate insomnia, restless legs, or circadian issues.
What are the most common concerns, and what should they know?
Many worry they will not sleep, but clinicians can still get useful data even if sleep is shorter than usual. Others worry the equipment will hurt, but sensors are designed to be non-invasive and safe.
Some also assume snoring always equals apnoea, which is not always true. A sleep study is helpful because it separates simple snoring from clinically significant breathing disruption that needs treatment.
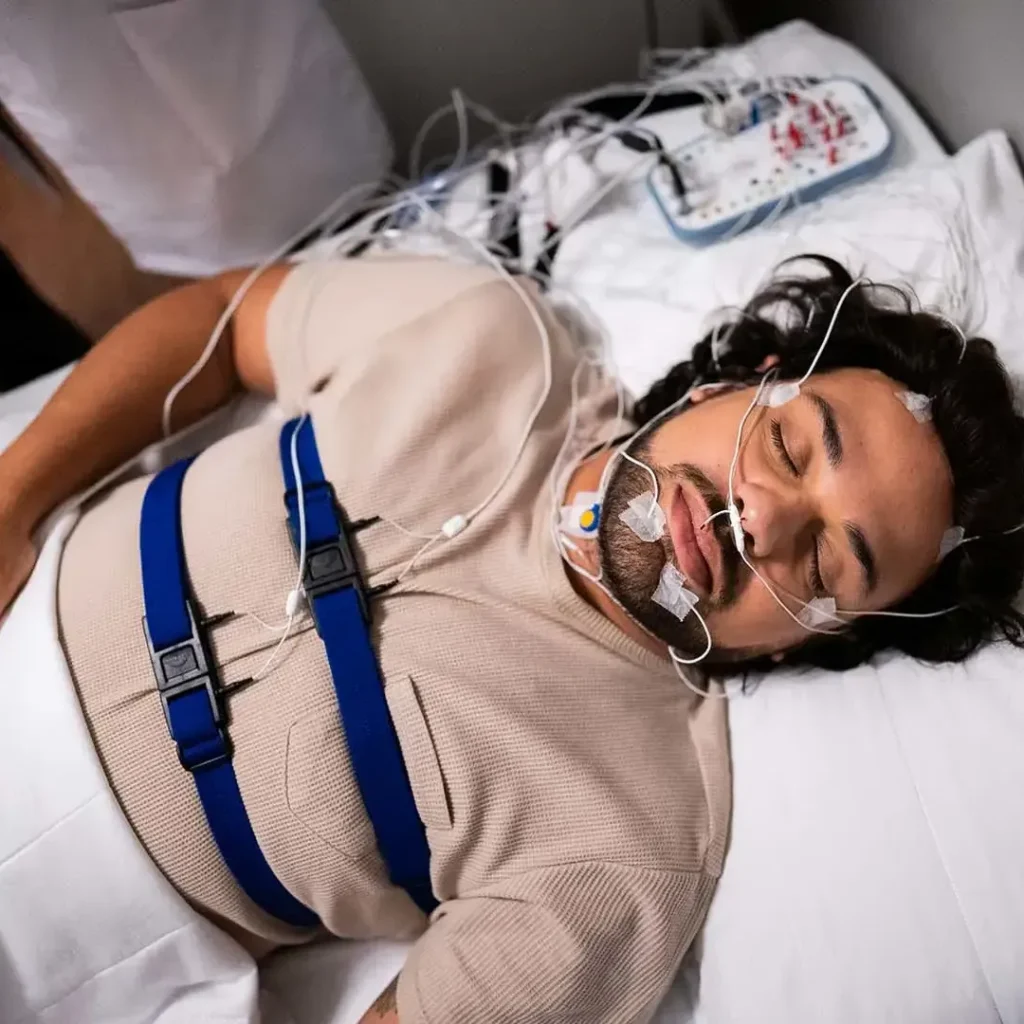
How can they make sure their sleep study is as accurate as possible?
They should follow setup instructions carefully and try to sleep as normally as possible. For home studies, correct placement of sensors and keeping the device on overnight are the biggest factors.
They should also tell the clinician about typical sleep habits, alcohol use, medications, and nasal congestion, since those can affect breathing. If the night was unusual, they should mention it so the report is interpreted in context.
FAQs (Frequently Asked Questions)
What is a sleep study in Adelaide and what does it measure?
A sleep study in Adelaide records key body signals overnight to help clinicians diagnose sleep issues. It measures airflow, oxygen levels, breathing effort, heart rate, body position, and snoring. More comprehensive studies also track brain activity and sleep stages to identify problems like obstructive sleep apnoea, insomnia, or movement disorders.
Who should consider undergoing a sleep study in Adelaide?
Individuals experiencing symptoms such as loud snoring, choking or gasping at night, witnessed breathing pauses, morning headaches, or persistent daytime sleepiness should consider a sleep study. It is also relevant for people with high blood pressure, type 2 diabetes, weight gain where sleep apnoea is suspected, or those with fatigue-related driving risks or work safety concerns.
How do I know if I need a home sleep study or an in-lab sleep study?
The choice depends on your symptoms and medical history. Home sleep studies are suitable when obstructive sleep apnoea is strongly suspected without complex health issues. In-lab studies are better for those with significant heart or lung disease, suspected central sleep apnoea, unusual movements during sleep, possible narcolepsy, or unclear prior tests. In-lab studies capture more detailed signals including sleep stages.
What should I expect during a home sleep study?
During a home sleep study in Adelaide, you will wear a small portable device overnight that includes sensors like a nasal cannula for airflow, a finger probe for oxygen levels, and belts around the chest or abdomen to measure breathing effort. You’ll set up the equipment before bed and return it the next day. Although done at home for comfort, some sensors may take getting used to.
How can I prepare for my sleep study to ensure accurate results?
To prepare for your sleep study in Adelaide, aim for a typical day by avoiding naps and limiting caffeine later in the day. Avoid alcohol as it can worsen snoring and apnoea. Follow medication instructions from your clinician and keep skin clean and dry to help sensors stick properly. For in-lab studies, bring comfortable sleepwear and any usual nighttime devices like mouthguards.
What happens after my sleep study and how long until I get results?
Sleep study results usually take from a few days up to two weeks depending on the clinic. A sleep physician reviews the data and you may have a follow-up appointment to discuss findings. If obstructive sleep apnoea is diagnosed, treatment options include CPAP therapy, oral appliances, weight management support, positional therapy, or referral to an ENT specialist. If no apnoea is found, other issues like insomnia or restless legs may be investigated.
Related: Is a Home Sleep Study Brisbane Better Than In-Clinic Testing?